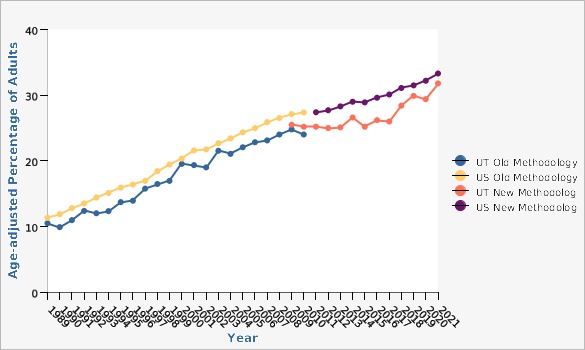
PHOM Indicator Profile Report of Obesity Among Adults
Why Is This Important?
Obesity can be costly and serious. Adults who are obese have an increased risk of hypertension, high LDL cholesterol, type 2 diabetes, coronary heart disease, stroke, and osteoarthritis.Obesity in the U.S. and in Utah continues to increase.
Data Sources
- Behavioral Risk Factor Surveillance System Survey Data, US Department of Health and Human Services Centers for Disease Control and Prevention (CDC).
- The Utah Department of Health and Human Services Behavioral Risk Factor Surveillance System (BRFSS)
Data Notes
Obesity is defined as a body mass index (BMI) of 30 or more. BMI is calculated by dividing weight in kilograms by the square of height in meters. [[br]]Age-adjusted to U.S. 2000 standard population.[[br]] [[br]]U.S. data does not include U.S. territories, but does include Dist. of Columbia.[[br]] [[br]] Beginning in 2011, BRFSS data include both landline and cell phone respondent data along with a new weighting methodology called iterative proportional fitting, or raking. Comparisons between 2011 and prior years should be made with caution. More details about these changes can be found at: [https://ibis.health.utah.gov/pdf/opha/resource/brfss/RakingImpact2011.pdf].Risk Factors
There are things that people can do that can reduce their risk of obesity. Behaviors such as engaging in physical activity and having a healthy diet can have a significant impact on reducing the risk (see [https://www.cdc.gov/obesity/adult/causes.html/ Centers for Disease Control and Prevention, Overweight & Obesity: Adult Obesity Causes & Consequences.]).How Are We Doing?
The age-adjusted percentage of Utah adults (18+) who were obese increased from 19.5% in 2000 to 31.8% in 2021. Nevertheless, Utah still has a lower obesity rate than most states. A release from CDC (2022) maps prevalence by state. See [http://www.cdc.gov/obesity/data/prevalence-maps.html/ Adult Obesity Prevalence Maps].What Is Being Done?
The Utah Department of Health and Human Service's Healthy Environments Active Living (HEAL) Program plays a key role in improving the health of residents in the state of Utah. The program was formed in July 2013 (as Healthy Living through Environment, Policy, and Improved Clinical Care: EPICC), through a new funding opportunity from the Centers of Disease Control and Prevention (CDC) that allowed for the merging of three previously existing programs: the Heart Disease and Stroke Prevention Program, the Diabetes Prevention and Control Program, and the Physical Activity, Nutrition and Obesity Program, as well as the addition of a school health program. HEAL was recently restructured as part of a strategic planning process and the new program model focuses on staff and partners working together to address the social determinants of health while advancing health equity and increasing policy, systems and environmental changes. HEAL works: In schools:[[br]] HEAL encourages schools to adopt the Comprehensive School Physical Activity Program. This framework encourages students to be physically active for 60 minutes a day through school, home, and community activities. HEAL also tracks height and weight trends in elementary school students. In worksites:[[br]] HEAL offers training on developing worksite wellness programs called Work@Health. HEAL partners with local health departments to encourage worksites to complete the CDC Scorecard and participate in yearly health risk assessments for their employees. HEAL provides toolkits and other resources for employers interested in implementing wellness programs [https://heal.health.utah.gov/worksite-wellness/ Worksite Wellness]. In communities:[[br]] HEAL receives federal funding to partner with worksites and community-based organizations to increase access to fresh fruits and vegetables in worksite and community settings. HEAlL also partners with LHDs to work with cities and/or counties within their jurisdictions to create a built environment that encourages physical activity. In healthcare:[[br]] HEAL works with health care systems to establish community clinical linkages to support individuals at risk for or diagnosed with diabetes or hypertension to engage in lifestyle change programs such as chronic disease self-management and diabetes prevention programs. In childcare:[[br]] HEAL works with state and local partners through the Childcare Obesity Prevention workgroup to implement policy and systems changes in early care and education across agencies statewide. Ten local health departments statewide have implemented the TOP Star program, which aims to improve the nutrition, physical activity, and breastfeeding policies and environments and achieve best practices in childcare centers and homes.[[br]]Healthy People Objective: Reduce the proportion of adults who are obese
U.S. Target: 30.5 percentState Target: 24.0 percent