Why Is This Important?
The number of overweight or obese children and adolescents is increasing and diseases previously thought to affect mainly adults, such as type 2 diabetes, high blood pressure, and high cholesterol, are now being diagnosed in children and adolescents. The social and psychological impacts of childhood obesity include social isolation, increased rate of suicidal thoughts, low self-esteem, increased rate of anxiety disorders and depression, and increased likelihood of being bullied.Percentage of Utah Children Who Were Obese by Grade and Sex, 1st, 3rd, and 5th Grades, Utah, 2018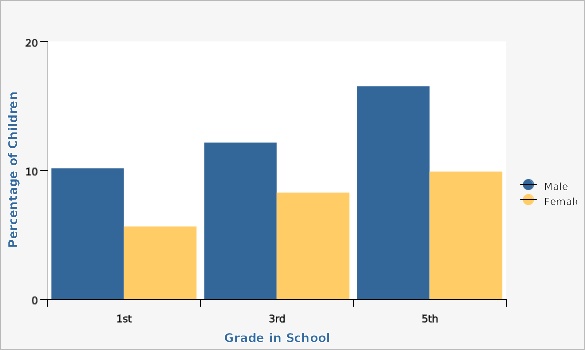 |
Data Source
Utah Department of Health, Bureau of Health Promotion, Healthy Living Through Environment, Policy and Improved Clinical Care Program Height/Weight Measurement
Data Notes
Childhood obesity is determined by calculating BMI using the height, weight, age, and sex of the child. The child is considered to be obese if the resulting BMI is greater than or equal to the 95th percentile for age and sex based on the Centers for Disease Control and Prevention Growth Charts (2 to 20 years: Boys Body Mass index-for-age percentiles and 2 to 20 years: Girls Body Mass index-for-age percentiles). [[br]]
[[br]] In 2018 height and weight measurements were collected from 3,944 1st, 3rd, and 5th grade students in 69 randomly selected public elementary schools in Utah.How Are We Doing?
The percentage of obese children in Utah increased dramatically in the first decade of the century. From 1994 to 2010 the number of obese third grade boys increased by 97 percent, from 6.0 percent in 1994 to 11.8 percent in 2010. The percentage of obese third grade girls increased by 40 percent over the same time period. In 2010, 8.4 percent of third grade girls were obese compared to 6.0 percent in 1994. Childhood obesity in Utah seems to have leveled off since 2010. In 2018, 12.1% of third grade boys and 8.3% of girls were obese.
Among adolescents in 2019, 9.3 percent of Utah public high school students were obese; boys were over twice as likely as girls to be obese (13.2% compared to 6.3%). The adolescent obesity rate nationally is considerably higher than Utah's rate, where 14.8% of U.S. adolescents were obese in 2017.
The obesity rate in 2019 among adolescents in grades 8, 10, and 12 was lower in Summit County (4.7%, Tri-County (4.7%), and Utah County (8.6%) than the state rate (9.8%). The obesity rate among adolescents in grades 8, 10, and 12 was higher in Weber-Morgan (12.1%) and Tooele (12.2%) than the state rate.
Adolescent obesity rates varied dramatically by race and ethnicity. According to the 2017 Prevention Needs Assessment data Pacific Islanders (29.1%), Native Americans (15.9%), Blacks (15.2%), and Hispanics (13.9%) in grades 8, 10, and 12 all had higher rates of obesity than the state rate (9.6%). White adolescents (8.1%) had lower rates than the state rate.
It is likely that these data, based on self-reported height and weight, underrepresent the prevalence of overweight or obesity among high school students.What Is Being Done?
The Healthy Living through Environment, Policy, and Improved Clinical Care Program (EPICC) was established through funding from the Centers for Disease Control and Prevention (CDC).
EPICC focuses on Environmental Approaches that Promote Health, specifically promoting policies around healthy eating and active living. EPICC works:
In Schools:[[br]]
1) Schools are encouraged to adopt the Comprehensive School Physical Activity Program. This framework encourages students to be physically active for 60 minutes a day through school, home and community activities.[[br]]
2) Height and weight trends are being tracked in a sample of elementary students to monitor Utah students.[[br]]
3) Action for Healthy Kids brings partners together to improve nutrition and physical activity environments in Utah's schools by implementing the school-based state plan strategies, working with local school boards to improve or develop policies for nutritious foods in schools. This includes recommendations for healthy vending options.
In Communities:[[br]]
1) Local health departments (LHDs) receive federal funding to partner with schools, worksites, and other community based organizations to increase access to fresh fruits and vegetables through food service guidelines, farmers markets, and retail stores. LHDs also work with cities within their jurisdictions to create a built environment that encourages physical activity.
In Healthcare:[[br]]
1) EPICC works with health care systems to establish community clinical linkages to support individuals at risk for or diagnosed with diabetes or hypertension to engage in lifestyle change programs such as chronic disease self-management and diabetes prevention programs.
In Childcare:[[br]]
1) Ten local health departments statewide have implemented the TOP Star program, which aims to improve the nutrition, physical activity, and breastfeeding environments and achieve best practice in child care centers and homes.[[br]]
2) EPICC works with state and local partners through the Childcare Obesity Prevention workgroup to implement policy and systems changes in early care and education across agencies statewide.Healthy People Objective: Reduce the proportion of children and adolescents who are considered obese
U.S. Target: Not applicable, see subobjectives in this category
Date Indicator Content Last Updated: 10/27/2020
Other Views
- by Grade and Sex, 1st, 3rd, and 5th Grades, Utah, 2018
- by Grade and Sex, Grades 9-12, Utah, 2019
- Grades 9-12, Utah and U.S., 1999-2019
- by Local Health District, Grades 8, 10, and 12, Utah, 2019

