Complete Health Indicator Report of Foodborne Illness - Shiga Toxin-producing ''E. coli'' (STEC) Infections
Definition
Number of reported culture-confirmed and probable cases of infections caused by Shiga toxin-producing ''Escherichia coli'' O157:H7 and non-O157 serogroups per 100,000 population per year.Numerator
Number of reported culture-confirmed and probable cases of infections caused by Shiga toxin-producing ''Escherichia coli'' O157:H7 and non-O157 serogroups per year.Denominator
Total Utah population per year.Data Interpretation Issues
The Utah Department of Health and Human Services tracks one category of ''E. coli'' that causes diarrhea, known as Shiga toxin-producing ''E. coli'' or STEC. These bacteria are sometimes referred to as enterohemorrhagic ''E. coli'' or EHEC. The most common strain of STEC is O157:H7, but there are many other strains of ''E. coli'' that produce Shiga toxin. Rather than listing all of them individually, all strains of ''E. coli'' that produce Shiga toxin are referred to as STEC.Why Is This Important?
All age groups can be infected with Shiga toxin-producing ''E. coli'' (STEC), but young children, the elderly, and those with compromised immune systems are the most severely affected. STEC are very common bacteria that can cause diarrheal illness in humans. The illness can range from mild to severe, bloody diarrhea. These infections cause approximately 100,000 illnesses, 3,000 hospitalizations, and about 90 deaths annually in the United States. The bacteria live in the intestines of some healthy cattle, and contamination of meat can occur in the slaughtering process. Eating ground beef that has been inadequately cooked is a common way of becoming infected. Other sources of infection may include drinking unpasteurized (raw) milk or juice; drinking or swimming in water that is contaminated with sewage or animal waste; eating contaminated fruits or vegetables; or contact with animals that are infected. Severe manifestations of STEC infection (HUS or TTP) require a prolonged hospital stay and may result in renal failure and death. Effective prevention is the best treatment for STEC.How Are We Doing?
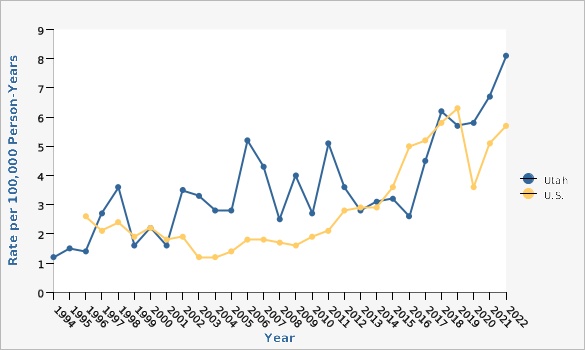
''E. coli'' O157:H7 infections became reportable in Utah in 1990; at that time, six cases were reported. The increase in the number of cases reported annually since 1990 may be due to improved reporting and better laboratory detection methods. Utah data for 2022 shows the incidence of STEC in Utah was at 8.1 cases per 100,000 person-years. STEC rates have risen over the last few years.How Do We Compare With the U.S.?
''Escherichia coli'' O157:H7 has been nationally notifiable since 1994. National surveillance for all Shiga toxin-producing ''E. coli'' (STEC), under the name enterohemorrhagic ''E. coli'' (EHEC), began in 2001. As of January 1, 2006, the nationally notifiable diseases case definition designation changed from EHEC to STEC, and serotype-specific reporting was implemented.What Is Being Done?
Per the Communicable Disease Rule R386-702-3, health care providers and laboratories are required to report cases of Shiga toxin-producing ''E. coli'' to the Office of Communicable Diseases or the local health department. The Disease Response, Evaluation, Analysis, and Monitoring (DREAM) Program at the Utah Department of Health and Human Services assists local health departments with the investigation of cases and outbreaks and implementation of control measures to prevent further cases. Because diagnosis solely on the basis of detection of Shiga toxin does not sufficiently protect the public's health, characterizing STEC isolates by serotype and whole-genome sequencing (WGS) is critical to detect, investigate, and control outbreaks. Screening of stool specimens by clinical diagnostic laboratories for Shiga toxin by culture independent diagnostic tests, and forwarding enrichment broths from Shiga toxin-positive specimens that do not yield STEC O157 to state or local public health laboratories are important for public health surveillance of all STEC infections. Local health departments attempt to interview every case of Shiga toxin-producing ''E. coli'' infection reported to public health. Information gathered during these interviews includes food history, water exposure, animal exposure, travel history, outdoor history, and contact with ill individuals. Data from these interviews are analyzed and used to identify outbreaks and common sources of infection. In addition, patients are provided with information on high-risk exposures and how to prevent future STEC infection in themselves and their families. [[br]][[br]] ''E. coli''-related illness can be prevented by following general guidelines, including: Practice proper hygiene, especially good handwashing. *Wash your hands thoroughly after using the bathroom and changing diapers. *Wash your hands thoroughly before and after preparing or eating food. *Wash your hands thoroughly after contact with animals or their environments (at farms, petting zoos, fairs, even your own backyard). *Wash your hands thoroughly before preparing and feeding bottles or foods to an infant or toddler, before touching an infant or toddler's mouth, and before touching pacifiers or other things that go into an infant or toddler's mouth. [[br]] Keep all objects that enter infants' and toddlers' mouths (such as pacifiers and teethers) clean. *If soap and water aren't available, use an alcohol-based hand sanitizer with at least 60% alcohol (check the product label to be sure). These alcohol-based products can quickly reduce the number of germs on hands in some situations, but they are not a substitute for washing with soap and running water. *Follow the four steps to food safety when preparing food: clean, separate, cook, and chill. *Wash fruits and vegetables well under running water, unless the package says the contents have already been washed. [[br]] Cook meats thoroughly. *To kill harmful germs, cook beef steaks and roasts to an internal temperature of at least 145F (62.6C) and allow to rest for 3 minutes after you remove meat from the grill or stove. *Cook ground beef and pork to a minimum internal temperature of 160F (70C). *Always use a food thermometer to check that the meat has reached a safe internal temperature because you can't tell whether meat is safely cooked by looking at its color. *Don't cause cross-contamination in food preparation areas. Thoroughly wash hands, counters, cutting boards, and utensils after they touch raw meat. *Avoid raw milk, unpasteurized dairy products, and unpasteurized juices (such as fresh apple cider). *Don't swallow water when swimming and when playing in lakes, ponds, streams, swimming pools, and backyard kiddie pools. [[br]] Visit [https://www.cdc.gov/ecoli/ecoli-prevention.html] for additional information.Available Services
Foodborne disease outbreaks and other outbreaks are investigated primarily by local health departments in collaboration with Utah Department of Health and Human Services as needed. For more information regarding local health departments in Utah, visit: [http://www.ualhd.org/] To report a foodborne illness, pelase visit: [http://igotsick.health.utah.gov]Related Indicators
Related Relevant Population Characteristics Indicators:
Related Health Care System Factors Indicators:
Risk Factors
All age groups can be infected with STEC, but young children, the elderly, and those with compromised immune systems are the most severely affected.Related Risk Factors Indicators:
Graphical Data Views
Rate of Reported STEC Infections Utah and U.S., 1994-2022
| Utah vs. U.S. | Year | Rate per 100,000 Person-Years | ||||
|---|---|---|---|---|---|---|
Record Count: 56 | ||||||
| Utah | 1994 | 1.2 | ||||
| Utah | 1995 | 1.5 | ||||
| Utah | 1996 | 1.4 | ||||
| Utah | 1997 | 2.7 | ||||
| Utah | 1998 | 3.6 | ||||
| Utah | 1999 | 1.6 | ||||
| Utah | 2000 | 2.2 | ||||
| Utah | 2001 | 1.6 | ||||
| Utah | 2002 | 3.5 | ||||
| Utah | 2003 | 3.3 | ||||
| Utah | 2004 | 2.8 | ||||
| Utah | 2005 | 2.8 | ||||
| Utah | 2006 | 5.2 | ||||
| Utah | 2007 | 4.3 | ||||
| Utah | 2008 | 2.5 | ||||
| Utah | 2009 | 4.0 | ||||
| Utah | 2010 | 2.7 | ||||
| Utah | 2011 | 5.1 | ||||
| Utah | 2012 | 3.6 | ||||
| Utah | 2013 | 2.8 | ||||
| Utah | 2014 | 3.1 | ||||
| Utah | 2015 | 3.2 | ||||
| Utah | 2016 | 2.6 | ||||
| Utah | 2017 | 4.5 | ||||
| Utah | 2018 | 6.2 | ||||
| Utah | 2019 | 5.7 | ||||
| Utah | 2020 | 5.8 | ||||
| Utah | 2021 | 6.7 | ||||
| Utah | 2022 | 8.1 | ||||
| U.S. | 1996 | 2.6 | ||||
| U.S. | 1997 | 2.1 | ||||
| U.S. | 1998 | 2.4 | ||||
| U.S. | 1999 | 1.9 | ||||
| U.S. | 2000 | 2.2 | ||||
| U.S. | 2001 | 1.8 | ||||
| U.S. | 2002 | 1.9 | ||||
| U.S. | 2003 | 1.2 | ||||
| U.S. | 2004 | 1.2 | ||||
| U.S. | 2005 | 1.4 | ||||
| U.S. | 2006 | 1.8 | ||||
| U.S. | 2007 | 1.8 | ||||
| U.S. | 2008 | 1.7 | ||||
| U.S. | 2009 | 1.6 | ||||
| U.S. | 2010 | 1.9 | ||||
| U.S. | 2011 | 2.1 | ||||
| U.S. | 2012 | 2.8 | ||||
| U.S. | 2013 | 2.9 | ||||
| U.S. | 2014 | 2.9 | ||||
| U.S. | 2015 | 3.6 | ||||
| U.S. | 2016 | 5.0 | ||||
| U.S. | 2017 | 5.2 | ||||
| U.S. | 2018 | 5.8 | ||||
| U.S. | 2019 | 6.3 | ||||
| U.S. | 2020 | 3.6 | ||||
| U.S. | 2021 | 5.1 | ||||
| U.S. | 2022 | 5.7 | ||||
Data Notes
Utah rates are derived from Utah annual surveillance reports published by the Office of Communicable Diseases. The U.S. rates are derived from the Centers for Disease Control Foodborne Diseases Active Surveillance Network (FoodNet). Utah and U.S. data are preliminary and may change. The CSTE case definition includes all confirmed and probable cases of STEC.Data Sources
- Utah Department of Health and Human Services Office of Communicable Diseases
- Population Estimates for 1999 and earlier: Utah Governor's Office of Planning and Budget
- For years 2020 and later, the population estimates are provided by the Kem C. Gardner Policy Institute, Utah state and county annual population estimates are by single year of age and sex, IBIS Version 2022
- Population Estimates for 2000-2019: National Center for Health Statistics (NCHS) through a collaborative agreement with the U.S. Census Bureau, IBIS Version 2020
- U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC)
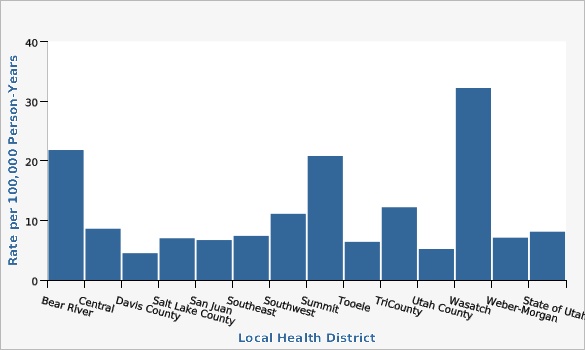
Reported Confirmed and Probable STEC Infections by Local Health District, Utah, 2022
| Local Health District | Rate per 100,000 Person-Years | |||||
|---|---|---|---|---|---|---|
Record Count: 14 | ||||||
| Bear River | 21.8 | |||||
| Central | 8.6 | |||||
| Davis County | 4.5 | |||||
| Salt Lake County | 7.0 | |||||
| San Juan | 6.7 | |||||
| Southeast | 7.4 | |||||
| Southwest | 11.1 | |||||
| Summit | 20.8 | |||||
| Tooele | 6.4 | |||||
| TriCounty | 12.2 | |||||
| Utah County | 5.2 | |||||
| Wasatch | 32.2 | |||||
| Weber-Morgan | 7.1 | |||||
| State of Utah | 8.1 | |||||
Data Notes
Utah rates are derived from Utah annual surveillance reports published by the Office of Communicable Diseases. Includes all reported confirmed and probable Shiga toxin-producing ''E. coli'' (STEC) cases.Data Sources
- Utah Department of Health and Human Services Office of Communicable Diseases
- For years 2020 and later, the population estimates are provided by the Kem C. Gardner Policy Institute, Utah state and county annual population estimates are by single year of age and sex, IBIS Version 2022
- U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC)
References and Community Resources
Information for the general public from the Office of Communicable Diseases can be found by visiting: [https://epi.health.utah.gov/] Information for national rates of STEC infection can be found at: [https://wonder.cdc.gov/nndss/nndss_annual_tables_menu.asp] and at [https://wwwn.cdc.gov/foodnetfast/]More Resources and Links
Evidence-based community health improvement ideas and interventions may be found at the following sites:- Centers for Disease Control and Prevention (CDC) WONDER Database, a system for disseminating public health data and information.
- United States Census Bureau data dashboard.
- Utah healthy Places Index, evidence-based and peer-reviewed tool, supports efforts to prioritize equitable community investments, develop critical programs and policies across the state, and much more.
- County Health Rankings
- Kaiser Family Foundation's StateHealthFacts.org
- Medical literature can be queried at PubMed library.
Page Content Updated On 02/08/2024,
Published on 03/06/2024
