Complete Health Indicator Report of Maternal Mortality
Definition
'''Maternal mortality''' is a general term referring to the death of a woman during pregnancy or within a year of the end of pregnancy. Maternal deaths are also known as pregnancy-associated deaths. A '''pregnancy-related death''' is defined as the death of a woman during pregnancy or within one year of the end of pregnancy from a pregnancy complication, a chain of events initiated by pregnancy, or the aggravation of an unrelated condition by the physiologic effects of pregnancy. Pregnancy-related deaths are a subset of all pregnancy-associated (maternal) deaths. The '''pregnancy-related mortality ratio''' is the number of pregnancy-related deaths per 100,000 live births.Numerator
Number of pregnancy-related deaths per yearDenominator
Total number of live births per yearData Interpretation Issues
The CDC Pregnancy Mortality Surveillance System and the data presented here include pregnancy-related deaths during pregnancy and up to 365 days after the end of a pregnancy. The World Health Organization and Healthy People 2030 define a maternal death as the death of a woman while pregnant or within 42 days of the end of a pregnancy, from a pregnancy-related cause. Care should be taken to clarify whether data are based on a 42 day or 365 day time period and whether data refer to pregnancy-related deaths or pregnancy-associated (maternal) deaths.Why Is This Important?
More than 1200 women died in the United States as a result of their pregnancy or delivery complications in 2021 (CDC). The death of a woman during pregnancy, delivery, or after delivery is a tragedy for her family and for society as a whole. Surveillance of maternal mortality identifies ways to improve one's health, health behaviors, and health care before, during, and after pregnancy. Surveillance also identifies gaps in the health care system, social services, health care access, and the quality of prenatal and postnatal care.Other Objectives
Healthy People 2030 Objective MICH-04 aims to reduce the maternal mortality rate to 15.7 maternal deaths per 100,000 live births. This measure uses the definition of death while pregnant or within 42 days of being pregnant related to obstetric causes.How Are We Doing?
The Utah pregnancy-related mortality ratio for 2019-2021 was 20.8 pregnancy-related deaths per 100,000 live births.How Do We Compare With the U.S.?
Comparison between Utah and U.S. rates is complicated by differences in methodology when defining pregnancy-relatedness. As can be seen in the graph, the U.S. maternal mortality ratio has slowly increased. Reasons for this increase are not clear. Some of the increase is likely due to improved identification of maternal deaths. Other possible reasons may include an increase in chronic diseases that impact maternal health, including hypertension, diabetes, heart disease, and mental health conditions that put a person at higher risk of morbidity and mortality during pregnancy or in the year postpartum. Women may also experience more barriers to accessing affordable health care, which may increase health risks during and after pregnancy. More detailed information can be found at [https://www.cdc.gov/reproductivehealth/maternal-mortality/pregnancy-mortality-surveillance-system.htm].What Is Being Done?
The Utah Department of Health and Human Services conducts ongoing maternal mortality surveillance through the Perinatal Mortality Review program. Public education is provided on the importance of planning for pregnancy, preconception and interconception health, and recognition and treatment of maternal anxiety and depression. The Utah Women and Newborns Quality Collaborative (UWNQC) addresses issues of quality improvement in maternal and infant health care. The Hear Her campaign raises awareness of the urgent maternal warning signs during and after pregnancy to improve communication between patients, families, and healthcare providers. Utah has distributed more than 8,000 magnets with the urgent maternal warning signs to clinics, providers, and individuals attending community events.Evidence-based Practices
Utah collaborates with the Alliance for Innovation on Maternal Health (AIM) to promote consistent and safe maternity care. The AIM has developed patient safety bundles, a package of evidence-based best practices for implementation in clinical settings. Safety bundles address the leading causes of maternal mortality and are designed to reduce maternal deaths related to obstetrical complications. In 2020 and 2021, Utah worked on the implementation of the Obstetric Care for Women with Opioid Use Disorder bundle. In 2020, a new website was launched to make it easier to find a mental health care provider with expertise in perinatal mental health. This resource can be found at [http://maternalmentalhealth.utah.gov/]. Thirty-four Utah hospitals earned the "Birthing-Friendly" designation from the Centers for Medicare and Medicaid Services (CMS) in 2023. This designation describes high-quality maternity care. Learn more about the "Birthing-Friendly" designation and see a map of the Utah "Birthing-Friendly" hospitals at [https://data.cms.gov/provider-data/birthing-friendly-hospitals-and-health-systems].Available Services
Find providers trained in perinatal mental health based on provider type, location or insurance accepted at [https://maternalmentalhealth.utah.gov/]. Postpartum Support International-Utah provides extensive resources for maternal mental health. Visit their website at [https://www.psiutah.org/]. The University of Utah SUPeRAD clinic specializes in care for pregnant women with substance addictions. Call 801-581-8425 for more information. The University of Utah Huntsman Mental Health Institute specializes in perinatal mental health care for those experiencing perinatal mood and anxiety disorders, birth trauma, pregnancy loss, infertility, and having a baby in the NICU (neonatal intensive care unit). For more information call 801-585-1565 or visit their website at [https://healthcare.utah.edu/hmhi/treatments/perinatal-mental-health]. To find local substance use disorder and mental health treatment options, visit [https://sumh.utah.gov].Related Indicators
Related Relevant Population Characteristics Indicators:
Related Health Care System Factors Indicators:
Risk Factors
Nationally, Black women have a 3-4 times higher rate of pregnancy-related mortality than White women. Women aged 35 years or over are also at increased risk for pregnancy-related deaths. Women who received no prenatal care also had a higher risk of pregnancy-related mortality compared to those who received adequate prenatal care.Related Risk Factors Indicators:
Graphical Data Views
Pregnancy-related mortality ratio, Utah and U.S., 2007-2021
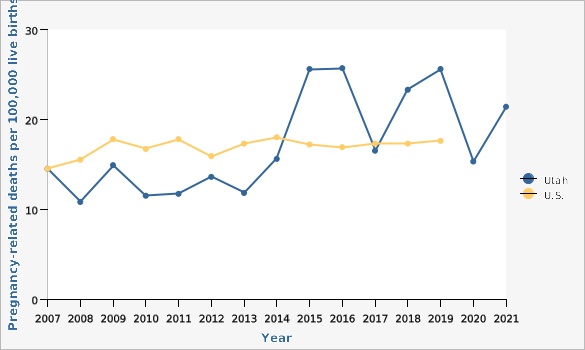
The final determination about whether a death is categorized as pregnancy-related is made by the Utah Maternal Mortality Review Committee. Over time the composition of the committee and the information available has changed, affecting how deaths are categorized. In 2015, the committee began using standardized criteria to determine when an overdose or suicide death was related to the pregnancy. These criteria were published in 2020 (Standardized Criteria for Review of Perinatal Suicides and Accidental Drug-Related Deaths, Smid, et al, [http://pubmed.ncbi.nlm.nih.gov/32925616/]). Because the total number of maternal deaths is low, the change in categorization for even one death may affect the mortality ratio.
| Utah vs. U.S. | Year | Pregnancy-related deaths per 100,000 live births | ||||
|---|---|---|---|---|---|---|
Record Count: 28 | ||||||
| Utah | 2007 | 14.5 | ||||
| Utah | 2008 | 10.8 | ||||
| Utah | 2009 | 14.9 | ||||
| Utah | 2010 | 11.5 | ||||
| Utah | 2011 | 11.7 | ||||
| Utah | 2012 | 13.6 | ||||
| Utah | 2013 | 11.8 | ||||
| Utah | 2014 | 15.6 | ||||
| Utah | 2015 | 25.6 | ||||
| Utah | 2016 | 25.7 | ||||
| Utah | 2017 | 16.5 | ||||
| Utah | 2018 | 23.3 | ||||
| Utah | 2019 | 25.6 | ||||
| Utah | 2020 | 15.3 | ||||
| Utah | 2021 | 21.4 | ||||
| U.S. | 2007 | 14.5 | ||||
| U.S. | 2008 | 15.5 | ||||
| U.S. | 2009 | 17.8 | ||||
| U.S. | 2010 | 16.7 | ||||
| U.S. | 2011 | 17.8 | ||||
| U.S. | 2012 | 15.9 | ||||
| U.S. | 2013 | 17.3 | ||||
| U.S. | 2014 | 18.0 | ||||
| U.S. | 2015 | 17.2 | ||||
| U.S. | 2016 | 16.9 | ||||
| U.S. | 2017 | 17.3 | ||||
| U.S. | 2018 | 17.3 | ||||
| U.S. | 2019 | 17.6 | ||||
Data Notes
Maternal deaths are identified through the pregnancy checkbox or cause of death codes on death certificates, or by matching birth and death certificates. The Utah Maternal Mortality Review Committee then determines whether each maternal death was related to the pregnancy or not. Deaths determined to be pregnancy-related are included in the pregnancy-related mortality ratio reported here. [[br]] [[br]] The U.S. data shown are from the CDC Pregnancy Mortality Surveillance System (PMSS), which summarizes and analyzes maternal death certificates and matching fetal death/birth certificates from 52 reporting areas. Maternal mortality data reported by PMSS are not yet available for years after 2019. [https://www.cdc.gov/reproductivehealth/maternal-mortality/pregnancy-mortality-surveillance-system.htm] The U.S. data presented here are most comparable to the Utah data, however, the case identification and classification methodologies differ slightly.Data Sources
- Office of Vital Records and Statistics, Utah Department of Health and Human Services
- Pregnancy Mortality Surveillance System, Division of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion
References and Community Resources
Pregnancy-Related Deaths - CDC.[[br]] [https://www.cdc.gov/hearher/pregnancy-related-deaths/index.html] Building U.S. Capacity to Review and Prevent Maternal deaths. Zaharatos, et al., Journal of Women's Health, Vol. 27, No. 1, 2018.[[br]] [https://pubmed.ncbi.nlm.nih.gov/29240525/] Global, regional, and national levels of maternal mortality, 1990-2015. Kassebaum, et al., Lancet. 2016 Oct 8;388 (10053):1775-1812. [[br]] [https://www.ncbi.nlm.nih.gov/pubmed/27733286] Standardized Criteria for Review of Perinatal Suicides and Accidental Drug-Related Deaths. Smid, et al., Obstetrics & Gynecology. 2020; 136(4):645-653. [[br]] [https://pubmed.ncbi.nlm.nih.gov/32925616/]More Resources and Links
Evidence-based community health improvement ideas and interventions may be found at the following sites:- Centers for Disease Control and Prevention (CDC) WONDER Database, a system for disseminating public health data and information.
- United States Census Bureau data dashboard.
- Utah healthy Places Index, evidence-based and peer-reviewed tool, supports efforts to prioritize equitable community investments, develop critical programs and policies across the state, and much more.
- County Health Rankings
- Kaiser Family Foundation's StateHealthFacts.org
- Medical literature can be queried at PubMed library.
Page Content Updated On 02/21/2024,
Published on 04/08/2024
