Why Is This Important?
Colorectal cancer is the third most commonly diagnosed cancer and the third most common cause of cancer-related death in both men and women in the United States.^1^
The U.S. Preventive Services Task Force recommends that routine screening for colorectal cancer begin at age 45 for adults at average risk. Persons at high risk may need to begin screening at a younger age. Routine screening can include either an annual fecal occult blood test (gFOBT or FIT), a flexible sigmoidoscopy every five years, a colonoscopy every 10 years, or a double-contrast barium enema every 5 to 10 years.
[[br]]
[[br]]
----
1. American Cancer Society, Colorectal Cancer Facts & Figures 2023-2025 Accessed at: [https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/colorectal-cancer-facts-and-figures/colorectal-cancer-facts-and-figures-2023.pdf].[[br]]
2. Centers for Disease Control and Prevention, Colorectal Cancer Screening Tests [https://www.cdc.gov/cancer/colorectal/basic_info/screening/tests.htm#:~:text=How%20often%3A%20Every%2010%20years,increased%20risk%20of%20colorectal%20cancer).].[[br]]Colorectal Cancer Deaths by Year, Utah and U.S., 1999-2022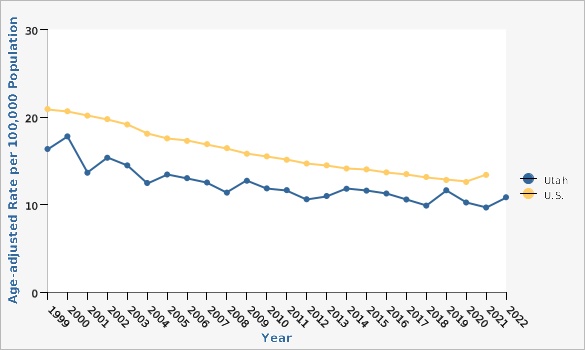 |
Data Sources
- Utah Death Certificate Database, Office of Vital Records and Statistics, Utah Department of Health and Human Services
- Population Estimates for 1999 and earlier: Utah Governor's Office of Planning and Budget
- For years 2020 and later, the population estimates are provided by the Kem C. Gardner Policy Institute, Utah state and county annual population estimates are by single year of age and sex, IBIS Version 2022
- Population Estimates for 2000-2019: National Center for Health Statistics (NCHS) through a collaborative agreement with the U.S. Census Bureau, IBIS Version 2020
- U.S. Cancer Statistics: WONDER Online Database. United States Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute. Accessed at [http://wonder.cdc.gov/cancer.html]
- National Vital Statistics System, National Center for Health Statistics, U.S. Centers for Disease Control and Prevention
Data Notes
ICD-10 codes used to define colorectal cancer: C18-C21.
Age-adjusted to U.S. 2000 standard population using 11 age adjustment age groups: (0, 1-4, 5-14, 15-24, 25-34, 35-44, 45-54, 55-64,65-74, 75-84, 85+).Risk Factors
Risk factors for colorectal cancer include increasing age, inflammatory bowel disease, a family history of polyps or colorectal cancer, a personal history of polyps or colorectal cancer, and certain hereditary syndromes. Physical inactivity, a low fiber/high fat diet, obesity, excessive alcohol consumption, and tobacco use may all increase risk. A diet high in fruits and vegetables, hormone replacement therapy in post-menopausal women, and aspirin use may reduce colorectal cancer risk.How Are We Doing?
The Utah colorectal cancer mortality rate has decreased significantly, from 17.8 deaths per 100,000 population in the year 2000 to 10.8 deaths per 100,000 population in 2022. Although overall mortality rates have decreased over time, mortality rates vary by age, sex, geography, ethnicity, and race. Looking at data from combined years 2020-2022, rates of colorectal cancer death significantly increase with age for both males and females. Males have higher rates of colorectal cancer deaths than females across all age groups. From 2018 to 2022 combined data, San Juan Local Health District (LHD) had the highest colorectal cancer mortality rate of 16.8 deaths per 100,000 population, while Davis County LHD had the lowest rate with 8.9 deaths per 100,000 population. Other geographical distribution of colorectal cancer deaths can also be viewed in more detail at the Utah Small Area level (see additional data views).
For combined years 2018-2022, there was no significant difference in colorectal cancer death rates between those of Hispanic (8.9 deaths per 100,000 population) and non-Hispanic ethnicity (10.7 deaths per 100,000 population). During the same time period, those who identified racially as Pacific Islander/Native Hawaiian had significantly higher colorectal cancer death rates (21.4 deaths per 100,000 population) compared to the overall mortality rate in Utah (10.6 deaths per 100,000 population).What Is Being Done?
Screening for colorectal cancer has recently been identified by the Centers for Disease Control and Prevention (CDC) as a priority public health issue.
Date Indicator Content Last Updated: 01/05/2024
Other Views
- by Year, Utah and U.S., 1999-2022
- by Age and Sex, Utah, 2020-2022
- by Local Health District, Utah, 2018-2022
- by Utah Small Area, 2018-2022
- by Ethnicity, Utah, 2018-2022
- by Race, Utah, 2018-2022

