PHOM Indicator Profile Report of Cesarean delivery among low risk women with no prior births
Why Is This Important?
The World Health Organization (WHO) defines normal birth as "...spontaneous in onset, low risk at the start of labor and remaining so throughout labor and delivery. The infant is born spontaneously in the vertex position between 37 and 42 completed weeks of pregnancy. After birth, mother and infant are in good condition." The aim of the care in normal birth is "to achieve a healthy mother and child with the least possible level of intervention that is compatible with safety. In normal birth, there should be a valid reason to interfere with the natural process." In 1970, the United States had a cesarean delivery rate of 5%. This increased to 20.8% in 1997, and to 32.1% in 2021, when nearly one-third of all children in the U.S. were born by cesarean delivery. The increases are present in all age groups and for all races and ethnic origins, without identified concurrent sources of increased obstetrical risk. A controversial aspect of this discussion is cesarean delivery on maternal request (CDMR) at term for a singleton pregnancy in the absence of any medical or obstetrical indication. It is not possible to obtain a confident estimate of the rate of CDMR at this time. Since a cesarean delivery entails major surgery for the mother, the following complications may occur (and may occur at a greater rate than for vaginal delivery): postpartum hemorrhage, infection, operative injury, thromboembolism, hysterectomy, anesthetic complications, placental problems in subsequent pregnancies (including placenta previa and accreta), postpartum depression, and increased risk of surgical complications in the presence of maternal obesity. Effects of cesarean delivery on the newborn may include difficulty with the initiation of breastfeeding, prematurity and its sequelae, lacerations, and respiratory problems. Both mother and infant will experience longer and more costly hospital stays than after a normal vaginal delivery.Rate of cesarean births among low risk women with no prior births, Utah and U.S., 2013-2021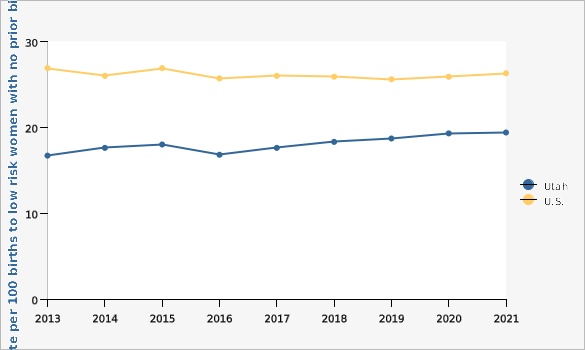 |
Data Sources
- Utah Birth Certificate Database, Office of Vital Records and Statistics, Utah Department of Health and Human Services
- National Vital Statistics System, National Center for Health Statistics, U.S. Centers for Disease Control and Prevention
Data Notes
[[br]]"Low risk" refers to women giving birth whose baby is term (37 weeks or greater), singleton (not a twin or other multiple-fetus pregnancy), and in the vertex or head down position.How Are We Doing?
In Utah, the rate of cesarean birth among low-risk women with no prior birth increased from 16.7% in 2013 to 19.4% in 2021, which is below the Healthy People 2030 objective.What Is Being Done?
The Utah Department of Health and Human Services has implemented the "Power Your Life" campaign to reach women of reproductive age about the importance of good health prior to pregnancy to improve outcomes. The centerpiece of the campaign is the Power Your Life website at http://poweryourlife.org/.Healthy People Objective: Reduce cesarean births among low-risk women with no prior cesarean births
U.S. Target: 23.9 percentState Target: 16.7 percent
