Why Is This Important?
Asthma can usually be managed in an outpatient setting, reducing the need for inpatient hospitalization. Tracking rates of hospitalization can aid in identifying populations or areas with inadequate access to routine medical care.
An asthma attack can result in hospitalization and can be initiated by a variety of triggers. Some of these include exposure to environmental tobacco smoke, dust mites, cockroach allergen, mold, pets, strenuous physical exercise, and air pollution. Two key air pollutants that can affect asthma are ozone (found in smog) and PM or particulate matter (found in haze, smoke, and dust).
The majority of problems associated with asthma, including hospitalization, are preventable if asthma is managed according to established guidelines. Effective management includes control of exposure to factors that trigger exacerbations, adequate pharmacological management, continual monitoring of the disease, and patient education in asthma care.Hospitalizations due to Asthma by Age Group, Utah, 2021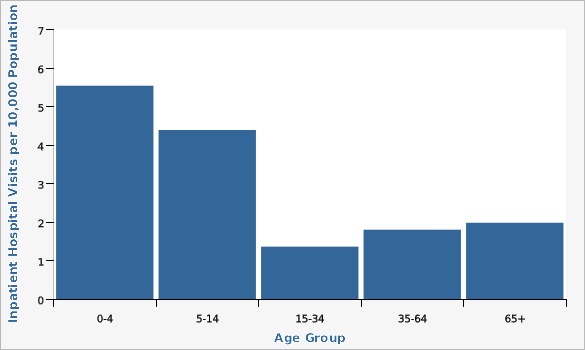 |
Data Source
Utah Inpatient Hospital Discharge Data, Office of Health Care Statistics, Utah Department of Health
Data Notes
Asthma was identified using the The National Center for Health Statistics (NCHS) 113 selected causes asthma definition.How Are We Doing?
In 2018-2019, Utah's overall age-adjusted hospitalization rate was 2.5 visits per 10,000 people. There are specific groups with a high number of hospitalizations due to asthma, these include males aged 0-4 (12.1 per 10,000 people) and females aged 0-4 (7.2 per 10,000 people).What Is Being Done?
The Utah Asthma Program (UAP) works with the Utah Asthma Task Force and other partners to maximize the reach, impact, efficiency, and sustainability of comprehensive asthma control services in Utah. This is accomplished by providing a seamless alignment of asthma services across the public health and health care sector, ensuring that people with asthma receive all of the services they need.
The UAP focuses on building program infrastructure and implementing strategies that improve asthma control, reduce asthma-related emergency department visits and hospitalizations, and reduce health care costs. Program infrastructure is strengthened through a focus on strategies to create and support a comprehensive asthma control program, these strategies include: strengthening leadership, building strategic partnerships, and using strategic communication, surveillance, and evaluation. In addition, the UAP implements strategies outlined in the Centers for Disease Control and Prevention (CDC) EXHALE technical package to improve asthma control. The six strategy areas outlined in the EXHALE technical package are:
1. Education on asthma self-management.
2. e-Xtinguishing smoking and secondhand smoke.
3. Home visits to trigger reduction and asthma self-management.
4. Achievement of guidelines-based medical management.
5. Linkages and coordination of care across settings.
6. Environmental policies or best practices to reduce asthma triggers from indoor, outdoor, and occupational sources.
These strategies are expected to improve asthma control and quality of life by increasing access to health care and increasing coordination and coverage for comprehensive asthma control services both in the public health and health care sectors. Specifically, these strategies include identifying people with poorly controlled asthma, linking them to health care providers and NAEPP EPR-3 guidelines-based care, educating them on asthma self-management strategies, providing a supportive school environment, and referring to or providing home trigger reduction services for those who need them.
Date Indicator Content Last Updated: 05/24/2023
Other Views
- by Age Group, Utah, 2021
- by Sex and Age, Utah, 2017-2019
- Crude Rates by Year, Utah, 2015-2021
- Counts by Year, Utah, 2016-2021
- Total Charges by Local Health District, Utah, 2019
- Average Charge per Visit by Local Health District, Utah, 2017-2019
- Age-adjusted Rates by Local Health District, Utah, 2017-2019
- Age-adjusted Rates by Year, Utah, 2015-2021

