Why Is This Important?
Asthma is a serious personal and public health issue that has far reaching medical, economic, and psychosocial implications. The burden of asthma can be seen in the number of asthma-related medical events, including emergency department visits, hospitalizations, and deaths.Asthma Prevalence Among Adults Aged 18 and Over, Utah and U.S., 2001-2021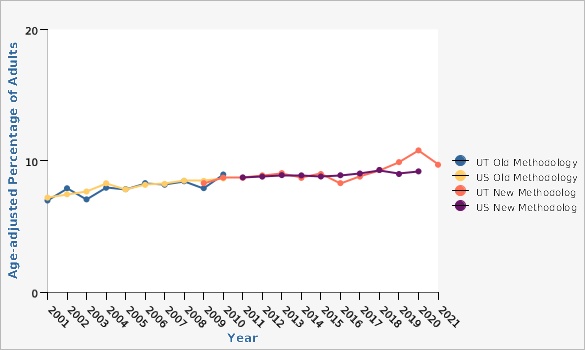 |
Data Sources
- Utah Department of Health and Human Services Behavioral Risk Factor Surveillance System (BRFSS) [https://ibis.health.utah.gov/ibisph-view/query/selection/brfss/BRFSSSelection.html]
- Behavioral Risk Factor Surveillance System Survey Data, US Department of Health and Human Services Centers for Disease Control and Prevention (CDC).
Data Notes
Rates have been age-adjusted to the U.S. 2000 standard population.
Note: At the time of this update, the BRFSS U.S. dataset did not include an age variable but did include five age categories up to age 80+ (vs. the typical weighting scheme that includes 85+). Comparisons with both weighting schemes were compared using Utah data, and the difference was about 1/100 of a percentage point.
In 2011, the BRFSS changed its methodology from a landline only sample and weighting based on post-stratification to a landline/cell phone sample and raking as the weighting methodology. Raking accounts for variables such as income, education, marital status, and home ownership during weighting and has the potential to more accurately reflect the population distribution.Risk Factors
People with respiratory diseases, including asthma, that make their lungs more vulnerable to ozone may experience health effects earlier and at lower ozone levels than other people. When ozone levels are high, more people with asthma have attacks that require a doctor's attention or use of medication. One reason this happens is that ozone makes people more sensitive to allergens such as pets, pollen, and dust mites, which are common triggers of asthma attacks.How Are We Doing?
Adult asthma rates show no sign of declining in Utah or in the U.S. In Utah and the U.S., adult asthma prevalence is higher for women than men in almost every age category.What Is Being Done?
The Utah Asthma Program (UAP) works with the Utah Asthma Task Force and other partners to maximize the reach, impact, efficiency, and sustainability of comprehensive asthma control services in Utah. This is accomplished by providing a seamless alignment of asthma services across the public health and health care sector, ensuring that people with asthma receive all of the services they need.
The UAP focuses on building program infrastructure and implementing strategies that improve asthma control, reduce asthma-related emergency department visits and hospitalizations, and reduce health care costs. Program infrastructure is strengthened through a focus on strategies to create and support a comprehensive asthma control program, these strategies include: strengthening leadership, building strategic partnerships, and using strategic communication, surveillance, and evaluation. In addition, the UAP implements strategies outlined in the Centers for Disease Control and Prevention (CDC) EXHALE technical package to improve asthma control. The six strategy areas outlined in the EXHALE technical package are:[[br]]
1. Education on asthma self-management.[[br]]
2. e-Xtinguishing smoking and secondhand smoke.[[br]]
3. Home visits for trigger reduction and asthma self-management.[[br]]
4. Achievement of guidelines-based medical management.[[br]]
5. Linkages and coordination of care across settings.[[br]]
6. Environmental policies or best practices to reduce asthma triggers from indoor, outdoor, and occupational sources.
These strategies are expected to improve asthma control and quality of life by increasing access to health care and increasing coordination and coverage for comprehensive asthma control services both in the public health and health care sectors. Specifically, these strategies include identifying people with poorly controlled asthma, linking them to health care providers and NAEPP EPR-3 guidelines-based care, educating them on asthma self-management strategies, providing a supportive school environment, and referring to or providing home trigger reduction services for those who need them.
Date Indicator Content Last Updated: 05/24/2023
Other Views
- by Disability, Utah Adults Aged 18 and Older, 2021
- Utah and U.S., 2001-2021
- by Age and Sex, Utah, 2021
- by Ethnicity, Utah, 2019-2021
- by Race, Utah, 2018-2021
- by Educational Level, Utah, 2020-2021
- by Income Level, Utah, 2020-2021
- by Utah Local Health District (2020-2021), Utah and U.S. (2020)
- by Local Health District, All Ages, Utah, 2020
- by Utah Small Area, 2016-2020

