Complete Health Indicator Report of Immunization - Influenza, adults
Definition
Number of adults who reported receiving an influenza vaccination in the past 12 months.Numerator
Number of survey respondents who reported receiving an influenza vaccination in the past 12 months.Denominator
Number of survey respondents.Data Interpretation Issues
Adult data for Utah and U.S. is also available from the FluVaxView Influenza Vaccination Coverage web page, which is estimated annually by CDC utilizing data from several nationally representative surveys. These surveys include the National Health Interview Survey (NHIS), the Behavioral Risk Factor Surveillance System (BRFSS), the National Immunization Survey (NIS), and in 2009-10, the National 2009 H1N1 Flu Survey (NHFS). For the 2010-11 influenza season, additional assessment systems were developed to provide timely coverage estimates for selected populations. These include: rapid household telephone surveys and cell phones conducted nationally and in 20 selected local areas, internet panel surveys of pregnant women and health care workers, and use of third-party medical claims data. Beginning in 2011, BRFSS data include both landline and cell phone respondent data along with a new weighting methodology called iterative proportional fitting, or raking. This methodology utilizes additional demographic information (such as education, race, and marital status) in the weighting procedure. Both of these methodology changes were implemented to account for an increased number of U.S. households without landline phones and an under-representation of certain demographic groups that were not well-represented in the sample. More details about these changes can be found at: [https://ibis.health.utah.gov/pdf/opha/resource/brfss/RakingImpact2011.pdf]. The survey question for this measure changed in 2011 to "During the past 12 months, have you had either a seasonal flu shot or a flu vaccine that was sprayed into your nose?". In previous years the question was "A flu shot is an influenza vaccine injected in your arm. During the past 12 months, have you had a seasonal flu shot?".Why Is This Important?
Influenza, or flu, is an acute viral infection involving the respiratory tract that can occur in epidemics or pandemics. Influenza can cause a person, especially older persons, to be more susceptible to bacterial pneumonia. It was estimated that in the 2022/23 flu season, 31 million flu illnesses occurred in the U.S. resulting in 360,000 hospitalizations and 21,000 deaths. Among children, this season was classified as high severity.^1^ The annual direct medical costs (hospitalization, doctors office visits, medications, etc.) for influenza in adults are estimated at $8.7 billion including $4.5 billion for adult hospitalizations resulting from influenza-attributable illness. Influenza is also responsible for substantial indirect costs ($6.2 billion annually), mainly from lost productivity.^2^ __References__ #Centers for Disease Control and Prevention (CDC). ''2022-2023 Estimated Influenza Burden''. Retrieved from: [https://www.cdc.gov/flu/about/burden/2022-2023.htm] #Centers for Disease Control and Prevention (CDC). ''Workplace Health Promotion - Flu & Pneumonia''. Retrieved from: [http://www.cdc.gov/workplacehealthpromotion/health-strategies/flu-pneumonia/index.html]Other Objectives
[[br]] ===Healthy People 2030 related objectives:=== IID-09: Increase the proportion of people who get the flu vaccine every year[[br]] '''U.S. Target:''' 70.0 percent [[br]]How Are We Doing?
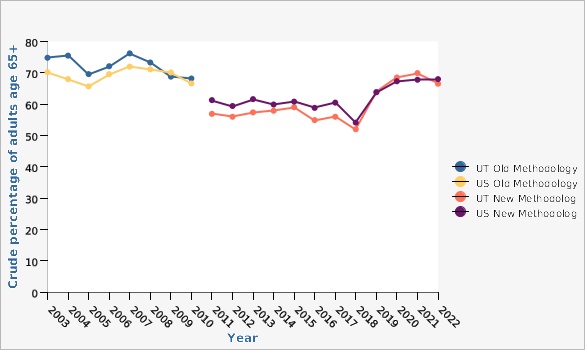
The percentage of Utahns aged 65+ who received a flu vaccine is measured by the Behavioral Risk Factor Surveillance System (BRFSS) survey, and was estimated to be 66.5% in 2022 as compared to 69.9% in 2021 and 68.5% in 2020. There was a decrease in coverage rates from 2007-2010 using the old BRFSS methodology and we saw a continuation of this decreased trend in 2011 and 2012 using the new methodology that was implemented in 2011. Using the new methodology, there was an increase in coverage rates from 2013-2015. Between 2018-2021 the rate increased from 52.0% and 69.9%. The rate then decreased by 3.4% in 2022 to 66.5%. Although this measure can fluctuate year to year, it is useful to observe the overall trends in the data.How Do We Compare With the U.S.?
In Utah, 66.5% of adults aged 65+ surveyed on the Behavioral Risk Factor Surveillance System (BRFSS) in 2022 reported receiving a flu shot in the previous 12 months. Nationwide for the same age group, the rate was 69.7%.What Is Being Done?
The DHHS Immunization Program and Office of Epidemiology educate health care providers, clinic staff, and the public about flu vaccination. ==Who Should Get Influenza Vaccine?== Everyone 6 months of age and older should get an flu vaccine every season with rare exception. For the 2023-2024 season, the Advisory Committee on Immunization Practices (ACIP) recommends annual influenza vaccination for everyone six months and older with any licensed, appropriate influenza vaccine with no preference expressed for any one vaccine over another. Some vaccines are not recommended in some situations and health conditions, and some people should not receive influenza vaccines at all (though this is uncommon). ===The Influenza (Flu) Shot=== ====People who can get the flu shot:==== *Different flu shots are approved for people of different ages. Everyone should get a vaccine that is appropriate for their age. *There are inactivated influenza vaccines that are approved for people as young as six months of age. *Some vaccines are only approved for adults. *Flu shots are recommended for pregnant women and people with chronic health conditions. [[br]] ====People who SHOULD NOT get the flu shot:==== *Children younger than six months of age are too young to get the flu shot. *People with severe, life-threatening allergies to flu vaccine or any ingredient in the vaccine. This might include gelatin, antibiotics, or other ingredients. [[br]] ====People who should talk to their doctor before getting the flu shot:==== If you have one of the following conditions, talk with your healthcare provider: *If you have an allergy to any of the ingredients in the vaccine. Talk to your doctor about your allergy. *If you ever had Guillain-Barr Syndrome (a severe paralyzing illness, also called GBS). Some people with a history of GBS should not get this vaccine. Talk to your doctor about your GBS history. *If you are not feeling well, talk to your doctor about your symptoms. [[br]] ===Nasal Spray Flu Vaccine=== ====People who can get the nasal spray flu vaccine:==== *The nasal spray vaccine is approved for use in people 2 years through 49 years of age. It is an option for healthy, non-pregnant people in this age group. [[br]] ====People who SHOULD NOT get the nasal spray vaccine:==== *Children younger than two years *Adults 50 years and older *Pregnant women *People with severe, life-threatening allergies to flu vaccine or any ingredient in the vaccine *Children 2 years through 17 years of age who are receiving aspirin- or salicylate- containing medications *People who are immunocompromised *Children 2 years through 4 years who have asthma or who have had a history of wheezing in the past 12 months *People who have taken influenza antiviral drugs within the previous 48 hours *People who care for severely immunocompromised persons who require a protected environment *People who have taken influenza antiviral drugs in the previous 48 hours [[br]] ====People who should talk to their healthcare provider:==== If you have one of the following conditions, talk with your healthcare provider. He or she can help decide whether vaccination is right for you, and then select the best vaccine for you situation: *People with asthma aged 5 years and older *People with other underlying medical conditions that can put them at high risk of developing serious flu complications. These include conditions such as chronic lung diseases, heart disease (except isolated hypertension), kidney disease, liver disorders, neurologic and neuromuscular disorders, blood disorders, or metabolic disorders (such as diabetes) *People with moderate or severe acute illness with or without fever *People with Guillain-Barr Syndrome within 6 weeks following a previous dose of influenza vaccine [[br]] __Reference__[[br]] Centers for Disease Control and Prevention (CDC). "Who Should and Who Should NOT get a Flu Vaccine". Retrieved from: [https://www.cdc.gov/flu/prevent/whoshouldvax.htm].Available Services
Available services for influenza include: * All influenza and pneumococcal vaccinations are covered for seniors with Medicare Part B. * Low-income and/or homeless adults can be immunized for a reduced fee based on income level at many Community Health Clinics. * Adults who are not U.S. citizens may also receive lower cost immunizations based on their income level at many Community Health Clinics. * Drive-by clinics are offered by some providers throughout the state for persons with limited physical mobility. * Immunizations can also be given to the home-bound through many private providers and county services. [[br]] Call the Immunization Hotline at 1-800-275-0659 for a list of Community Health Clinics, County Health Departments, Aging Services, and other providers who can assist you. Additionally, information about influenza and pneumococcal vaccinations can be found on the Utah Immunization Program website at: [https://immunize.utah.gov].Related Indicators
Relevant Population Characteristics
Age is a risk factor for influenza. Adults 65 years of age and older are at increased risk of contracting influenza due to a natural decline in the strength of their immune system. Children younger than five years, but especially younger than two years of age are considered high-risk for influenza. However, people of all ages with immune deficiencies or other high-risk conditions are at increased risk for influenza.Related Relevant Population Characteristics Indicators:
Health Care System Factors
All Health Insurance Marketplace plans and most other private insurance plans must cover influenza vaccines without charging a co-payment or co-insurance when provided by an in-network provider. This is true even for patients who have not met a yearly deductible. For older adults, Medicare part B does cover influenza and pneumococcal vaccinations, and Medicaid covers influenza and pneumococcal for children recommended to receive vaccine. A new long-term care facilities licensing rule has been implemented to guarantee consistent screening for influenza and pneumococcal vaccinations, for standing orders to give vaccines, for keeping immunization histories of all residents and employees, for the offer of a one-time pneumococcal vaccination for the residents, and for the annual offering of an influenza vaccination for both the residents and employees. This new rule should raise immunization rates for adults who reside in institutional settings.Related Health Care System Factors Indicators:
Risk Factors
Following is a list of all the health and age factors that are known to increase a person's risk of getting serious complications from flu: *Adults 65 years and older *Children younger than 2 years old **Although all children younger than 5 years old are considered at high risk for serious flu complications, the highest risk is for those younger than 2 years old, with the highest hospitalization and death rates among infants younger than 6 months old. *Asthma *Neurologic and neurodevelopment conditions *Blood disorders (such as sickle cell disease) *Chronic lung disease (such as chronic obstructive pulmonary disease [COPD] and cystic fibrosis) *Endocrine disorders (such as diabetes mellitus) *Heart disease (such as congenital heart disease, congestive heart failure and coronary artery disease) *Kidney diseases *Liver disorders *Metabolic disorders (such as inherited metabolic disorders and mitochondrial disorders) *People who are obese with a body mass index [BMI] of 40 or higher *People younger than 19 years old on long-term aspirin- or salicylate-containing medications. *People with a weakened immune system due to disease (such as people with HIV or AIDS, or some cancers such as leukemia) or medications (such as those receiving chemotherapy or radiation treatment for cancer, or persons with chronic conditions requiring chronic corticosteroids or other drugs that suppress the immune system) *People who have had a stroke [[br]] Other people at high risk from the flu: *Pregnant women and women up to 2 weeks after the end of pregnancy *People who live in nursing homes and other long-term care facilities *People from certain racial and ethnic minority groups are at increased risk for hospitalization with flu, including non-Hispanic Black persons, Hispanic or Latino persons, and American Indian or Alaska Native persons [[br]] __Reference__ #Centers for Disease Control and Prevention (CDC). ''People at High Risk For Flu Complications''. Retrieved from: [https://www.cdc.gov/features/fluhighrisk/index.html]Related Risk Factors Indicators:
Health Status Outcomes
Based on current recommendations for influenza and pneumococcal vaccines, any person with a risk factor for influenza or pneumonia should be screened by their health care provider for immunization status and be vaccinated. Any person with a risk factor for influenza or pneumonia who has been hospitalized for illness in the last year should have been immunized before leaving the hospital based on current recommendations, unless they decline vaccination or have a contraindication for receiving the vaccine. Any person with a risk factor for influenza or pneumonia who resides in a nursing home or long-term care facility should have received these immunizations upon entry into the facility based on current recommendations, unless declined or contraindicated. Since pneumonia is the most common serious complication of influenza, a pneumococcal vaccination could save their life.Related Health Status Outcomes Indicators:
Graphical Data Views
| BRFSS Utah vs. U.S. | Year | Crude percentage of adults age 65+ | Lower Limit | Upper Limit | ||
|---|---|---|---|---|---|---|
Record Count: 40 | ||||||
| UT Old Methodology | 2003 | 74.8% | 70.4% | 78.7% | ||
| UT Old Methodology | 2004 | 75.5% | 72.1% | 78.6% | ||
| UT Old Methodology | 2005 | 69.6% | 66.2% | 73.0% | ||
| UT Old Methodology | 2006 | 72.1% | 68.8% | 75.4% | ||
| UT Old Methodology | 2007 | 76.2% | 73.2% | 79.0% | ||
| UT Old Methodology | 2008 | 73.3% | 70.2% | 76.2% | ||
| UT Old Methodology | 2009 | 68.8% | 66.6% | 70.9% | ||
| UT Old Methodology | 2010 | 68.2% | 66.0% | 70.3% | ||
| US Old Methodology | 2003 | 70.2% | 70.2% | 70.2% | ||
| US Old Methodology | 2004 | 68.0% | 68.0% | 68.0% | ||
| US Old Methodology | 2005 | 65.7% | 65.7% | 65.7% | ||
| US Old Methodology | 2006 | 69.6% | 69.6% | 69.6% | ||
| US Old Methodology | 2007 | 72.0% | 72.0% | 72.0% | ||
| US Old Methodology | 2008 | 71.1% | 71.1% | 71.1% | ||
| US Old Methodology | 2009 | 70.1% | 70.1% | 70.1% | ||
| US Old Methodology | 2010 | 66.6% | 66.1% | 67.1% | ||
| UT New Methodology | 2011 | 56.9% | 54.6% | 59.1% | ||
| UT New Methodology | 2012 | 56.0% | 53.9% | 58.1% | ||
| UT New Methodology | 2013 | 57.4% | 55.1% | 59.7% | ||
| UT New Methodology | 2014 | 57.9% | 55.9% | 60.0% | ||
| UT New Methodology | 2015 | 59.0% | 56.4% | 61.4% | ||
| UT New Methodology | 2016 | 54.9% | 52.5% | 57.3% | ||
| UT New Methodology | 2017 | 56.0% | 53.5% | 58.4% | ||
| UT New Methodology | 2018 | 52.0% | 49.6% | 54.5% | ||
| UT New Methodology | 2019 | 63.9% | 61.7% | 65.9% | ||
| UT New Methodology | 2020 | 68.5% | 66.4% | 70.6% | ||
| UT New Methodology | 2021 | 69.9% | 67.7% | 72.0% | ||
| UT New Methodology | 2022 | 66.5% | 64.0% | 68.9% | ||
| US New Methodology | 2011 | 61.3% | 61.8% | 60.8% | ||
| US New Methodology | 2012 | 59.4% | 58.9% | 59.9% | ||
| US New Methodology | 2013 | 61.6% | 61.1% | 62.2% | ||
| US New Methodology | 2014 | 59.9% | 59.3% | 60.4% | ||
| US New Methodology | 2015 | 60.8% | 60.3% | 61.3% | ||
| US New Methodology | 2016 | 58.8% | 58.3% | 59.4% | ||
| US New Methodology | 2017 | 60.5% | 59.8% | 61.1% | ||
| US New Methodology | 2018 | 54.1% | 53.5% | 54.8% | ||
| US New Methodology | 2019 | 63.8% | 63.2% | 64.3% | ||
| US New Methodology | 2020 | 67.3% | 66.6% | 68.0% | ||
| US New Methodology | 2021 | 67.8% | 67.2% | 68.4% | ||
| US New Methodology | 2022 | 68.0% | 67.4% | 68.6% | ||
Data Notes
In 2011, the BRFSS changed its methodology from a landline only sample and weighting based on post-stratification to a landline/cell phone sample and raking as the weighting methodology. The data for 2011 and later on this graph are based on the new methodology (landline/cell phone sample; raking). Due to changes in both sampling and the question format, data for 2011 and later should be interpreted with caution compared to previous years. U.S. data are the average for all states and the District of Columbia; they do not include the U.S. territories. These rates are crude rates, not age-adjusted, given that the Healthy People 2030 Objective is based on crude rates.Data Sources
- Utah Department of Health and Human Services Behavioral Risk Factor Surveillance System (BRFSS) [https://ibis.health.utah.gov/ibisph-view/query/selection/brfss/BRFSSSelection.html]
- Behavioral Risk Factor Surveillance System Survey Data, US Department of Health and Human Services Centers for Disease Control and Prevention (CDC).
The survey question for this measure changed in 2011 to "During the past 12 months, have you had either a seasonal flu shot or a flu vaccine that was sprayed into your nose?". In previous years the question was "A flu shot is an influenza vaccine injected in your arm. During the past 12 months, have you had a seasonal flu shot?".
| Local Health District | Crude percentage of adults age 65+ | Lower Limit | Upper Limit | |||
|---|---|---|---|---|---|---|
Record Count: 15 | ||||||
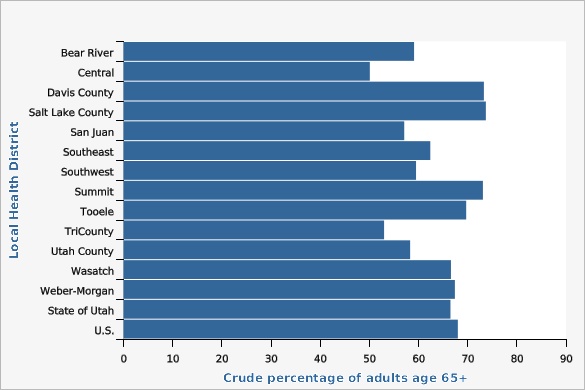
| Bear River | 59.1% | 48.7% | 68.7% | |||
| Central | 50.1% | 39.7% | 60.5% | |||
| Davis County | 73.3% | 65.1% | 80.1% | |||
| Salt Lake County | 73.7% | 69.3% | 77.8% | |||
| San Juan | 57.1% | 34.7% | 76.9% | |||
| Southeast | 62.4% | 50.2% | 73.3% | |||
| Southwest | 59.5% | 52.4% | 66.2% | |||
| Summit | 73.1% | 59.3% | 83.6% | |||
| Tooele | 69.7% | 57.5% | 79.7% | |||
| TriCounty | 53.0% | 42.5% | 63.2% | |||
| Utah County | 58.3% | 51.5% | 64.7% | |||
| Wasatch | 66.6% | 50.8% | 79.4% | |||
| Weber-Morgan | 67.4% | 58.6% | 75.2% | |||
| State of Utah | 66.5% | 64.0% | 68.9% | |||
| U.S. | 68.0% | 67.4% | 68.6% | |||
Data Notes
These rates are crude rates, not age-adjusted, given that the Healthy People 2030 Objective is based on crude rates. U.S. data are the average for all states and the District of Columbia; they do not include the U.S. territories.Data Sources
- Utah Department of Health and Human Services Behavioral Risk Factor Surveillance System (BRFSS) [https://ibis.health.utah.gov/ibisph-view/query/selection/brfss/BRFSSSelection.html]
- Behavioral Risk Factor Surveillance System Survey Data, US Department of Health and Human Services Centers for Disease Control and Prevention (CDC).
| Males vs. Females | Age Group | Crude percentage of adults | Lower Limit | Upper Limit | ||
|---|---|---|---|---|---|---|
Record Count: 12 | ||||||
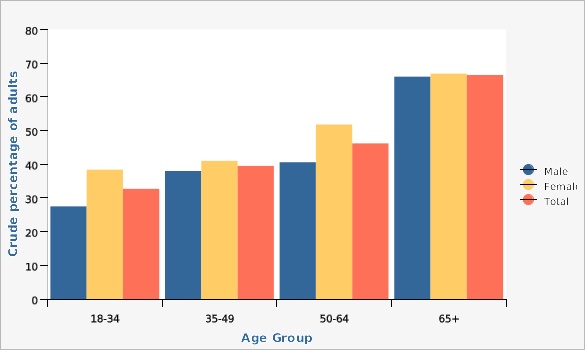
| Male | 18-34 | 27.5% | 24.3% | 31.0% | ||
| Male | 35-49 | 38.0% | 34.5% | 41.6% | ||
| Male | 50-64 | 40.6% | 36.8% | 44.5% | ||
| Male | 65+ | 66.0% | 62.5% | 69.3% | ||
| Female | 18-34 | 38.4% | 34.6% | 42.3% | ||
| Female | 35-49 | 41.0% | 37.5% | 44.6% | ||
| Female | 50-64 | 51.8% | 47.8% | 55.7% | ||
| Female | 65+ | 66.9% | 63.3% | 70.3% | ||
| Total | 18-34 | 32.7% | 30.2% | 35.3% | ||
| Total | 35-49 | 39.5% | 37.0% | 42.0% | ||
| Total | 50-64 | 46.2% | 43.4% | 49.0% | ||
| Total | 65+ | 66.5% | 64.0% | 68.9% | ||
Data Sources
- Utah Department of Health and Human Services Behavioral Risk Factor Surveillance System (BRFSS) [https://ibis.health.utah.gov/ibisph-view/query/selection/brfss/BRFSSSelection.html]
- Behavioral Risk Factor Surveillance System Survey Data, US Department of Health and Human Services Centers for Disease Control and Prevention (CDC).
| Race/Ethnicity Group | Crude percentage of adults age 18+ | Lower Limit | Upper Limit | |||
|---|---|---|---|---|---|---|
Record Count: 7 | ||||||
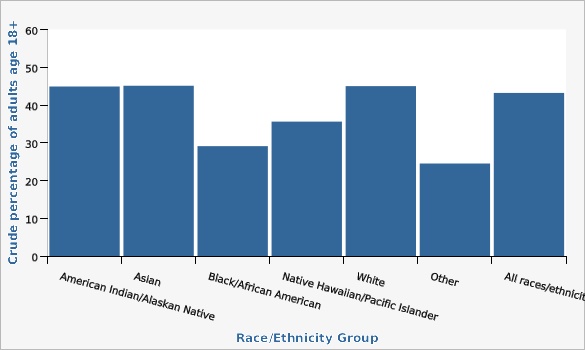
| American Indian/Alaskan Native | 44.9% | 33.2% | 57.3% | |||
| Asian | 45.1% | 36.0% | 54.6% | |||
| Black/African American | 29.1% | 19.7% | 40.8% | |||
| Native Hawaiian/Pacific Islander | 35.6% | 21.3% | 53.1% | |||
| White | 45.0% | 43.6% | 46.4% | |||
| Other | 24.5% | 20.1% | 29.5% | |||
| All races/ethnicities | 43.2% | 41.9% | 44.6% | |||
Data Notes
NOTE: INCLUDES ALL ADULTS 18+. These rates are crude rates, not age-adjusted, given that the Healthy People 2030 Objective is based on crude rates.Data Sources
- Utah Department of Health and Human Services Behavioral Risk Factor Surveillance System (BRFSS) [https://ibis.health.utah.gov/ibisph-view/query/selection/brfss/BRFSSSelection.html]
- Behavioral Risk Factor Surveillance System Survey Data, US Department of Health and Human Services Centers for Disease Control and Prevention (CDC).
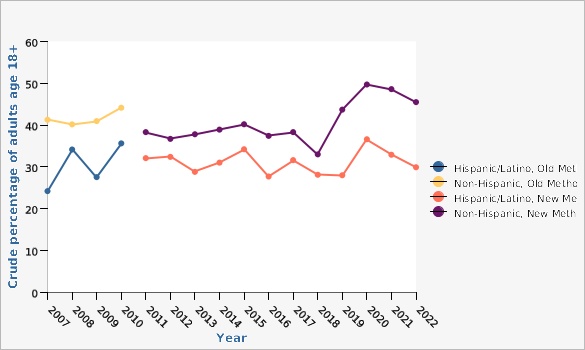
| Ethnicity and Methodology | Year | Crude percentage of adults age 18+ | Lower Limit | Upper Limit | ||
|---|---|---|---|---|---|---|
Record Count: 32 | ||||||
| Hispanic/Latino, Old Methodology | 2007 | 24.2% | 18.9% | 30.4% | ||
| Hispanic/Latino, Old Methodology | 2008 | 34.1% | 27.8% | 41.1% | ||
| Hispanic/Latino, Old Methodology | 2009 | 27.5% | 23.0% | 32.6% | ||
| Hispanic/Latino, Old Methodology | 2010 | 35.6% | 30.3% | 41.4% | ||
| Non-Hispanic, Old Methodology | 2007 | 41.3% | 39.3% | 43.2% | ||
| Non-Hispanic, Old Methodology | 2008 | 40.2% | 38.3% | 42.1% | ||
| Non-Hispanic, Old Methodology | 2009 | 41.0% | 39.5% | 42.4% | ||
| Non-Hispanic, Old Methodology | 2010 | 44.2% | 42.6% | 45.7% | ||
| Hispanic/Latino, New Methodology | 2011 | 32.1% | 28.2% | 36.2% | ||
| Hispanic/Latino, New Methodology | 2012 | 32.4% | 28.3% | 36.8% | ||
| Hispanic/Latino, New Methodology | 2013 | 28.8% | 25.1% | 32.9% | ||
| Hispanic/Latino, New Methodology | 2014 | 31.0% | 28.0% | 34.3% | ||
| Hispanic/Latino, New Methodology | 2015 | 34.2% | 30.4% | 38.2% | ||
| Hispanic/Latino, New Methodology | 2016 | 27.7% | 23.7% | 32.0% | ||
| Hispanic/Latino, New Methodology | 2017 | 31.6% | 27.9% | 35.6% | ||
| Hispanic/Latino, New Methodology | 2018 | 28.1% | 24.7% | 31.8% | ||
| Hispanic/Latino, New Methodology | 2019 | 28.0% | 24.7% | 31.5% | ||
| Hispanic/Latino, New Methodology | 2020 | 36.6% | 32.7% | 40.7% | ||
| Hispanic/Latino, New Methodology | 2021 | 32.9% | 29.5% | 36.5% | ||
| Hispanic/Latino, New Methodology | 2022 | 29.9% | 26.6% | 33.4% | ||
| Non-Hispanic, New Methodology | 2011 | 38.3% | 37.1% | 39.5% | ||
| Non-Hispanic, New Methodology | 2012 | 36.7% | 35.6% | 37.8% | ||
| Non-Hispanic, New Methodology | 2013 | 37.8% | 36.6% | 38.9% | ||
| Non-Hispanic, New Methodology | 2014 | 38.9% | 37.9% | 39.9% | ||
| Non-Hispanic, New Methodology | 2015 | 40.2% | 39.0% | 41.4% | ||
| Non-Hispanic, New Methodology | 2016 | 37.4% | 36.1% | 38.7% | ||
| Non-Hispanic, New Methodology | 2017 | 38.3% | 37.0% | 39.6% | ||
| Non-Hispanic, New Methodology | 2018 | 33.0% | 31.8% | 34.2% | ||
| Non-Hispanic, New Methodology | 2019 | 43.7% | 42.4% | 44.9% | ||
| Non-Hispanic, New Methodology | 2020 | 49.7% | 48.6% | 51.1% | ||
| Non-Hispanic, New Methodology | 2021 | 48.6% | 47.2% | 49.9% | ||
| Non-Hispanic, New Methodology | 2022 | 45.5% | 44.1% | 47.0% | ||
Data Notes
NOTE: INCLUDES ALL ADULTS 18+. In 2011, the BRFSS changed its methodology from a landline only sample and weighting based on post-stratification to a landline/cell phone sample and raking as the weighting methodology. The 2011-2022 data on this graph is based on the new methodology (landline/cell phone sample; raking). Due to changes in both sampling and the question format, data for 2011 and later should be interpreted with caution compared to previous years. These rates are crude rates, not age-adjusted, given that the Healthy People 2030 Objective is based on crude rates.Data Sources
- Utah Department of Health and Human Services Behavioral Risk Factor Surveillance System (BRFSS) [https://ibis.health.utah.gov/ibisph-view/query/selection/brfss/BRFSSSelection.html]
- Behavioral Risk Factor Surveillance System Survey Data, US Department of Health and Human Services Centers for Disease Control and Prevention (CDC).
References and Community Resources
More information on the Behavioral Risk Factor Surveillance System may be found on the website of the Centers for Disease Control and Prevention - [http://www.cdc.gov/brfss/] To find clinics that provide flu vaccine in your community, please utilize the HealthMap Vaccine Finder at: [https://www.vaccines.gov/find-vaccines/]More Resources and Links
Evidence-based community health improvement ideas and interventions may be found at the following sites:- Centers for Disease Control and Prevention (CDC) WONDER Database, a system for disseminating public health data and information.
- United States Census Bureau data dashboard.
- Utah healthy Places Index, evidence-based and peer-reviewed tool, supports efforts to prioritize equitable community investments, develop critical programs and policies across the state, and much more.
- County Health Rankings
- Kaiser Family Foundation's StateHealthFacts.org
- Medical literature can be queried at PubMed library.
Page Content Updated On 12/18/2023,
Published on 02/26/2024