Why Is This Important?
The infant mortality rate is an important measure of a nation's health and a worldwide indicator of health status and social well-being. The top four causes of infant mortality in Utah are perinatal conditions (including preterm birth), birth defects, medical conditions of the infant, and sudden unexpected infant death (SUID).Infant mortality: Deaths under 1 year of age, Utah and U.S., 1992-2022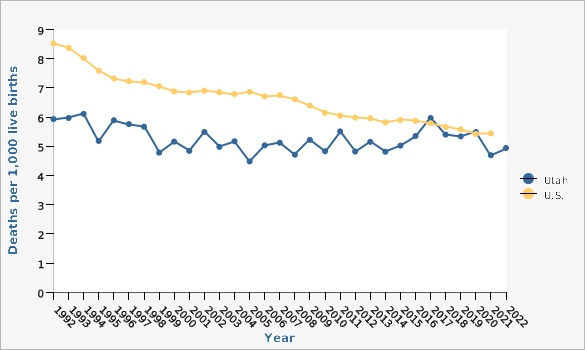 |
Data Sources
- Utah Death Certificate Database, Office of Vital Records and Statistics, Utah Department of Health and Human Services
- Utah Birth Certificate Database, Office of Vital Records and Statistics, Utah Department of Health and Human Services
- National Vital Statistics System, National Center for Health Statistics, U.S. Centers for Disease Control and Prevention
Data Notes
U.S. data from National Vital Statistics System [https://www.cdc.gov/nchs/products/databriefs/db456.htm#section_5].Risk Factors
Higher rates of infant mortality are noted among the following:
* Maternal inadequate weight gain during pregnancy
* Maternal pre-pregnancy BMI (obese prior to pregnancy)
* Maternal tobacco use
* Less than 6 months between pregnancies
* Infant birth weight (less than 2,500 g)
* Preterm infant
* Multiple gestation (e.g. twins)How Are We Doing?
The infant mortality rate has declined throughout the past 30 years both locally and nationally. The Utah infant mortality rate in 2022 was 4.9 deaths per 1,000 live births, similar to the 2021 infant mortality rate of 4.7. During 2022, 226 Utah infants died before their first birthday.What Is Being Done?
The Utah Department of Health and Human Services (DHHS) Maternal and Infant Health Program is currently reviewing data to identify modifiable risk factors for infant mortality, developing appropriate interventions, and promoting preconception and interconception health care for all reproductive aged women.
Date Indicator Content Last Updated: 02/21/2024

