Complete Health Indicator Report of Immunizations - Pneumonia, adults
Definition
Percentage of adults 65+ who reported receiving a pneumococcal vaccination at any point in their lifetime.Numerator
Number of survey respondents age 65+ who reported receiving a pneomococcal vaccine anytime during their life.Denominator
Number of survey respondents age 65+.Why Is This Important?
Pneumococcal disease is caused by bacteria that can spread from person to person through close contact. It can cause ear infections, and it can also lead to more serious infections of the lungs (pneumonia), blood (bacteremia), and covering of the brain and spinal cord (meningitis). Anyone can get pneumococcal disease, but children under two years of age and adults aged 65 years and older, people with certain medical conditions, and cigarette smokers are at the highest risk. [[br]] Before there was a vaccine, the United States saw: *More than 700 cases of meningitis *About 13,000 blood infections *About 5 million ear infections *About 200 deaths Treatment of pneumococcal infections with penicillin and other drugs is not as effective as it used to be, because some strains of pneumococcal are resistant to these drugs. This makes prevention of the disease, through immunization, even more important^1^. [[br]] ====Pneumococcal Vaccines==== There are three pneumococcal vaccines that are recommended for use in the United States: *Pneumococcal conjugate vaccine (PCV15/VAXNEUVANCE, PCV20/Prevnar 20) *Pneumococcal polysaccharide vaccine (PPSV23/Pneumovax23)[[br]] [[br]] The pneumococcal conjugate vaccines (PCV15/VAXNEUVANCE, PCV20/Prevnar 20) are recommended for: *Children at 2, 4, 6, and 12 through 15 months old and up to 5 years for those who missed doses *Adults 65 years or older *Children 5 years or older with certain medical conditions *Adults aged 18 to 64 years with certain medical conditions [[br]] The pneumococcal polysaccharide vaccine (PPSV23) is recommended for: *Children 2 through 18 years old with certain medical conditions *Adults who receive PCV15 *Adults who have received an earlier vaccine called PCV13^2^ [[br]] A 2006 study published in the medical journal Clinical Infectious Diseases found that hospital patients who received the pneumococcal vaccine were 40 to 70 percent less likely to die than unvaccinated patients. In the study, vaccinated patients had a lower risk of respiratory failure, kidney failure, heart attack, and other complications. Vaccinated patients in the study also spent an average of two fewer days in the hospital^3^.[[br]] [[br]] ---- 1. Centers for Disease Control and Prevention (CDC). "Pneumococcal Conjugate (PCV13) VIS. Retrieved from: [https://www.cdc.gov/vaccines/hcp/vis/vis-statements/pcv13.html] [[br]] 2. Centers for Disease Control and Prevention (CDC). ''Pneumococcal Vaccination: What Everyone Should Know'' Retrieved from: [https://www.cdc.gov/vaccines/vpd/pneumo/public/index.html][[br]] 3. Vila-Crcoles, et al. Protective Effects of the 23-Valent Pneumococcal Polysaccharide Vaccine in the Elderly Population: The EVAN-65 Study. ''Clinical Infectious Diseases''. Retrieved from: [http://cid.oxfordjournals.org/content/43/7/860.full]Other Objectives
[[br]] ===Healthy People 2030 related objectives:=== IID-D03: Increase the proportion of adults age 19 years or older who get recommended vaccines[[br]]How Are We Doing?
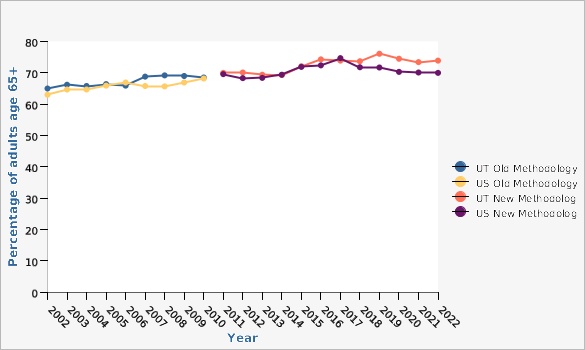
Lifetime pneumococcal vaccination rates for Utah adults 65+ have significantly improved since 1997 when data were first collected on the BRFSS. The 2001 rate was 67.3% and by 2020 the rate had increased to 74.5%. However, due to a change in the BRFSS methodology in 2011, it is not possible to know if this is a significant change. Rates have remained above 70% since 2015.How Do We Compare With the U.S.?
In 2022, the pneumococcal vaccination rate for adults age 65+ in the United States was 70.0%, while the Utah rate was 73.9%.Available Services
The Utah Immunization Program continues to administer the Adult High Risk (AHB) Initiative which provides the following vaccines for uninsured adults who are at risk for contracting hepatitis B: *Hepatitis A & B vaccine *Human Papillomavirus vaccine *Pneumococcal polysaccharide vaccine *Tetanus, diphtheria & pertussis vaccine [[br]] [[br]] Adults at high risk for contracting Hepatitis B may be able to access PPSV vaccine through this program.Related Indicators
Related Relevant Population Characteristics Indicators:
Related Health Care System Factors Indicators:
Related Risk Factors Indicators:
Graphical Data Views
Percentage of adults 65+ who reported having ever received pneumococcal vaccination, Utah and U.S., 2002-2022
| BRFSS Utah vs. U.S. | Year | Percentage of adults age 65+ | Lower Limit | Upper Limit | ||
|---|---|---|---|---|---|---|
Record Count: 42 | ||||||
| UT Old Methodology | 2002 | 65.0% | 60.3% | 69.7% | ||
| UT Old Methodology | 2003 | 66.2% | 61.4% | 71.0% | ||
| UT Old Methodology | 2004 | 65.8% | 62.1% | 69.5% | ||
| UT Old Methodology | 2005 | 66.4% | 62.9% | 69.9% | ||
| UT Old Methodology | 2006 | 65.9% | 62.4% | 69.4% | ||
| UT Old Methodology | 2007 | 68.8% | 65.4% | 72.0% | ||
| UT Old Methodology | 2008 | 69.2% | 65.9% | 72.2% | ||
| UT Old Methodology | 2009 | 69.0% | 66.7% | 71.2% | ||
| UT Old Methodology | 2010 | 68.5% | 66.3% | 70.6% | ||
| US Old Methodology | 2002 | 63.0% | 59.2% | 65.9% | ||
| US Old Methodology | 2003 | 64.7% | 61.8% | 68.6% | ||
| US Old Methodology | 2004 | 64.7% | 62.1% | 67.9% | ||
| US Old Methodology | 2005 | 65.9% | 62.5% | 69.2% | ||
| US Old Methodology | 2006 | 66.9% | 64.1% | 69.5% | ||
| US Old Methodology | 2007 | 65.8% | 65.2% | 66.4% | ||
| US Old Methodology | 2008 | 65.7% | 65.2% | 66.2% | ||
| US Old Methodology | 2009 | 66.9% | 66.4% | 67.4% | ||
| US Old Methodology | 2010 | 68.2% | 67.8% | 68.6% | ||
| UT New Methodology | 2011 | 70.0% | 67.8% | 72.2% | ||
| UT New Methodology | 2012 | 70.1% | 68.1% | 72.1% | ||
| UT New Methodology | 2013 | 69.4% | 67.2% | 71.6% | ||
| UT New Methodology | 2014 | 69.3% | 67.4% | 71.3% | ||
| UT New Methodology | 2015 | 72.1% | 69.6% | 74.4% | ||
| UT New Methodology | 2016 | 74.3% | 72.1% | 76.4% | ||
| UT New Methodology | 2017 | 73.9% | 71.5% | 76.1% | ||
| UT New Methodology | 2018 | 73.7% | 71.5% | 75.8% | ||
| UT New Methodology | 2019 | 76.1% | 74.2% | 77.9% | ||
| UT New Methodology | 2020 | 74.5% | 72.4% | 76.4% | ||
| UT New Methodology | 2021 | 73.4% | 71.2% | 75.4% | ||
| UT New Methodology | 2022 | 73.9% | 71.5% | 76.1% | ||
| US New Methodology | 2011 | 69.6% | 69.1% | 70.1% | ||
| US New Methodology | 2012 | 68.3% | 67.7% | 68.8% | ||
| US New Methodology | 2013 | 68.4% | 67.9% | 68.9% | ||
| US New Methodology | 2014 | 69.4% | 68.8% | 69.9% | ||
| US New Methodology | 2015 | 71.9% | 71.4% | 72.4% | ||
| US New Methodology | 2016 | 72.4% | 71.9% | 72.9% | ||
| US New Methodology | 2017 | 74.7% | 74.2% | 75.3% | ||
| US New Methodology | 2018 | 71.8% | 71.2% | 72.4% | ||
| US New Methodology | 2019 | 71.7% | 71.2% | 72.2% | ||
| US New Methodology | 2020 | 70.3% | 69.6% | 71.0% | ||
| US New Methodology | 2021 | 70.1% | 69.5% | 70.7% | ||
| US New Methodology | 2022 | 70.0% | 69.4% | 70.5% | ||
Data Notes
Beginning in 2011, BRFSS data include both landline and cell phone respondent data along with a new weighting methodology called iterative proportional fitting, or raking. This methodology utilizes additional demographic information (such as education, race, and marital status) in the weighting procedure. Both of these methodology changes were implemented to account for an increased number of U.S. households without landline phones and an under-representation of certain demographic groups that were not well-represented in the sample. More details about these changes can be found at: [https://ibis.health.utah.gov/pdf/opha/resource/brfss/RakingImpact2011.pdf]Data Sources
- Utah Department of Health and Human Services Behavioral Risk Factor Surveillance System (BRFSS) [https://ibis.health.utah.gov/ibisph-view/query/selection/brfss/BRFSSSelection.html]
- Behavioral Risk Factor Surveillance System Survey Data, US Department of Health and Human Services Centers for Disease Control and Prevention (CDC).
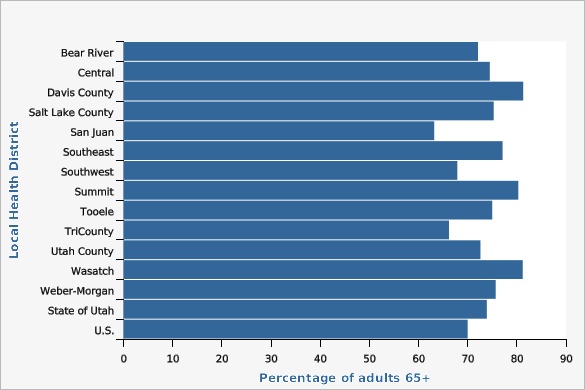
| Local Health District | Percentage of adults 65+ | Lower Limit | Upper Limit | Note | ||
|---|---|---|---|---|---|---|
Record Count: 15 | ||||||
| Bear River | 72.1% | 62.1% | 80.3% | |||
| Central | 74.5% | 64.9% | 82.1% | |||
| Davis County | 81.3% | 74.4% | 86.7% | |||
| Salt Lake County | 75.3% | 70.6% | 79.4% | |||
| San Juan | 63.2% | 39.1% | 82.2% | * | ||
| Southeast | 77.1% | 66.7% | 85.0% | |||
| Southwest | 67.9% | 60.6% | 74.4% | |||
| Summit | 80.3% | 67.2% | 89.0% | |||
| Tooele | 75.0% | 63.5% | 83.9% | |||
| TriCounty | 66.2% | 55.9% | 75.1% | |||
| Utah County | 72.6% | 66.2% | 78.2% | |||
| Wasatch | 81.2% | 68.6% | 89.6% | |||
| Weber-Morgan | 75.7% | 67.5% | 82.4% | |||
| State of Utah | 73.9% | 71.5% | 76.1% | |||
| U.S. | 70.0% | 69.4% | 70.5% | |||
Data Notes
*Use caution in interpreting; the estimate has a relative standard error greater than 30% and does not meet DHHS standards for reliability. Beginning in 2011, BRFSS data include both landline and cell phone respondent data along with a new weighting methodology called iterative proportional fitting, or raking. This methodology utilizes additional demographic information (such as education, race, and marital status) in the weighting procedure. Both of these methodology changes were implemented to account for an increased number of U.S. households without landline phones and an under-representation of certain demographic groups that were not well-represented in the sample. This graph is based on the new methodology. More details about these changes can be found at: [https://ibis.health.utah.gov/pdf/opha/resource/brfss/RakingImpact2011.pdf]Data Sources
- Utah Department of Health and Human Services Behavioral Risk Factor Surveillance System (BRFSS) [https://ibis.health.utah.gov/ibisph-view/query/selection/brfss/BRFSSSelection.html]
- Behavioral Risk Factor Surveillance System Survey Data, US Department of Health and Human Services Centers for Disease Control and Prevention (CDC).
More Resources and Links
Evidence-based community health improvement ideas and interventions may be found at the following sites:- Centers for Disease Control and Prevention (CDC) WONDER Database, a system for disseminating public health data and information.
- United States Census Bureau data dashboard.
- Utah healthy Places Index, evidence-based and peer-reviewed tool, supports efforts to prioritize equitable community investments, develop critical programs and policies across the state, and much more.
- County Health Rankings
- Kaiser Family Foundation's StateHealthFacts.org
- Medical literature can be queried at PubMed library.
Page Content Updated On 12/19/2023,
Published on 02/22/2024